Behavioural Health Consultants (BHCs)
Trigger warning: This column discusses suicide, depression, anxiety, grief, and terminal illness.
If you are in crisis right now, please call or text 988 (suicide crisis line) or
call the Mental Health Help Line at 1-877-303-2642. Help is available 24/7.
The peaceful waters of Sakinaw Lake BC - a serene view can be very relaxing. Photo by Kelly Allard
Disclosure: I serve as co-chair of the Palliser Friends of Medicare board. The views expressed in this column are my own; they do not represent the positions of that organization. Kelly Allard
One more thing before I start: Let's be honest about what people are carrying right now. Our province feels more divided than ever - the separation talks, the political anger, the sense that we are all picking sides. On top of that, many of us are watching what is happening in the Middle East and feeling helpless, scared, or heartbroken. Global conflict lands in our living rooms through our phones, and it stays with us. It is okay if you are feeling heavier than usual. You are not alone in that.
The Best-Kept Secret in Alberta Health Care (And Why We Need More of Them
In my last column I wrote about the parts of our health care system that feel like they are on fire. This time I want to talk about the part that is working. The part that, quite literally, held my family together.
I’m talking about Behavioural Health Consultants, or BHCs.
If you’ve never heard of them, you are not alone. They are Alberta Health Services' best-kept secret. They are free. You do not need a referral that takes months. They are available in person or over the phone, often within days - or even hours if things are really bad. The number of visits is unlimited and as often as you need, whether it is once a month or once a week.
They’re not psychiatrists so they don’t prescribe medication; they work with your family doctor who can. Think of them as a specialist for the everyday stresses: relationship struggles, grief, depression, anxiety, PTSD.
I know how good they are because one saved my husband's life, she also saved my sanity. She helped my whole family navigate the death of a loved one as well as other issues.
A Quiet Hero in the Palliser Zone
I live in the Palliser Health Zone. My family doctor is attached to the Primary Care Network (PCN) here. I have been seeing my BHC for about ten years. It started with my husband Carl in 2016, he was dealing with a Workers' Compensation Board (WCB) claim (his employer was absolutely awful about it). He fell into such a deep depression that I was afraid he might die by suicide. After he started seeing a BHC the improvement was steady, the positive change was remarkable.
“Before seeing a BHC”
Photo by Kelly Allard
Eventually I started seeing her too.
I was a real basket case at the time; my anxiety was through the roof. I mistakenly thought that talking to a counsellor was a sign of weakness (was I ever wrong!).
I didn't realize how bad it had gotten because I was just so used to surviving, the smallest setback could send me spiralling.
My BHC described it as “hanging on by the fingernails”.
Here’s some of what Carl and I had gone through over the years:
Carl - testicular cancer, a motorcycle wreck that almost killed him and eventually cost him his leg after two and a half years of surgeries, congestive heart failure (CHF) from a virus that enlarged his heart and ended up in a 9 day stint in the hospital, COPD, diabetes, a work injury that re-broke an old ankle fracture, reconstructive surgery on that ankle that took a year to heal from.
Me - two emergency C-sections, acute kidney failure from a medication resulting in a five-day hospital stay and 6 weeks of a urinary catheter (which severely curtailed my riding ability - plastic urine collection bags and hot pipes do not mix), chronic pain which required opiates for over 20 years.
It just kept coming, one thing after another. When Carl was diagnosed and then hospitalized with pulmonary embolisms in the summer of 2016 that ended his ability to work, I was overwhelmed. I was ultimately diagnosed with Caregiver PTSD. In retrospect I had symptoms for years - fatigue, anxiety, flashbacks, crying when talking about Carl’s health issues.
After seeing a BHC
Photo by Kelly Allard
It sneaks up on you.
You don't notice the damage because you're too busy putting out fires.
My BHC suggested medication at first, and I told her, "Let’s try talk therapy first."
It worked.
It was invaluable in late 2016 when my husband got the flu that sent him into septic shock and put him on life support for a month. During those weeks on life support amidst daily visits with an unconscious Carl, I put on a brave face for my family; I had to pretend everything was going to be okay. (They weren’t fooled.)
I saw my BHC once a week back then, I could tell her the fears I couldn't tell others. I could fall apart in private so I could stay strong in public. He survived, but I don't know how I would have survived with my sanity intact without her. While Carl had to learn to walk, talk and eat again, it helped him being able to speak with our BHC; he could talk to her about things he did not want to burden me with.
The next year, we found out Carl had terminal cancer. This time, the BHC was there for both of us. She helped us navigate the terror of the diagnosis and she later helped the rest of family.
This is the part I really like - because she knew all of us, she understood the family dynamic. She could see when one of us was being stubborn, avoiding the issue or just plain full of shit. She never told us what to do. She just helped us work out what we needed to do; sometimes, she called us out on our bullshit.
She helped us all talk about the hard stuff before he died, which made saying goodbye a tiny bit easier.
I still see her at least once a month, I saw her today in fact.
I do it for the same reason I take care of my physical health. With her help I was able to manage the chronic pain I have had for over 25 years, I was able to wean myself off the pain meds over 2 years ago. The pain is still there but I have learned to manage my stress which decreases my pain.
Mental Health Care is part of Health Care. The mind affects the body and can affect your physical health - anxiety and stress can raise your heart rate, your blood pressure, your pain, your blood sugars …
A Lesson in Being "Selfish"
Here is something else my BHC taught me that I think everyone needs to hear. At times when one of my adult kids was in crisis, I would offer to give up my appointment so they could have my spot. I thought I was being a good mom - sacrificing for my children.
My BHC eventually stopped me.
She reminded me that my kids were adults. Their mental health was their responsibility to manage. And my issues - the ones I was carrying from years of trauma and caregiving - were just as important as theirs. She taught me that I couldn't keep emptying myself for everyone else.
There is a saying up on the wall in my BHCs office:
"You cannot pour from an empty cup."
Caregivers do this all the time. We put ourselves last. We think our needs can wait. But if you are running on empty, you are no good to anyone - including yourself. Learning to be "selfish" about your own mental health? That’s not selfish at all. That’s survival; that’s strength.
Let Me Say It Again: It's Okay to Not Be Okay
I need to repeat something because it is so important, and we don't hear it enough.
It’s okay to not be okay
Asking for help is not a sign of weakness
Asking For Help is a sign of strength
I’ve had people in my life use me as their therapist. They dumped their troubles on me and expected me to help solve them.
It’s exhausting.
It drains you.
Thanks to my BHC, I’ve learned to set boundaries and to say “No”. I encourage them to get real help from a professional who is trained for this.
Here’s another hard lesson I learned: those drunken phone calls in the middle of the night. You know the ones. Someone calls you, slurring their words, telling you they are going to harm themselves unless you do something for them - stay on the phone, come over, fix their life. I used to think I had to save them. I would stay on the phone for hours, terrified they might actually do it.
But then they would call again the next time they got drunk and weepy.
And again.
And again.
Eventually, I learned to set a boundary - a serious one. I told them:
"If you tell me you are going to harm yourself, I will call 911 and get you the help you need."
The drunken phone calls stopped.
That doesn't mean I don't care. It means I care enough to take them seriously - and to recognize that I’m not equipped to handle a crisis. If someone is truly in danger, they need more than a friend on the phone. They need real help.
Venting with a friend is normal, I’m good with that. But if you are constantly carrying someone else's baggage, it wears you down. If you are the one doing the dumping, please know that your friends love you, but they might not be equipped to carry what you are carrying.
“Crocodile Dundee” once said that if people had more "mates," we wouldn't need to talk to professionals. Nice idea, but it's wrong - so wrong. My family and friends are wonderful, but some things are above their pay grade. My BHC has the training to guide me through the mess, not just listen to it. I don’t need to dump my trauma on my family and friends, it is unkind. Yes I might vent when faced with an irritant but they don’t need to hear about my entire life story.
This Makes Financial Sense
When people are struggling, the default is often to try to get in to see a psychiatrist but that is the wrong tool for the job most of the time. It’d be like seeing a heart surgeon because you have high blood pressure. Sure, the heart surgeon is a heart expert but in a different way. What you likely really need is a family doctor or a nurse to help you manage the condition with diet, exercise, and medication. The surgeon is for when things go really, really wrong - like when you need bypass surgery.
Psychiatrists are similar. They’re medical doctors who deal with severe mental illness: schizophrenia, bipolar disorder, major psychosis, etc. They’re absolutely necessary, but they’re also incredibly scarce. People wait months to see one.
BHCs fill the gap for the rest of us, the ones dealing with depression, anxiety, grief, and the everyday stresses of life. According to the Palliser Primary Care Network's latest plan, there are currently 8.5 full-time equivalent BHC positions working with family doctors in our zone. That's fewer than nine people covering a massive geographic area including Brooks, Oyen, Bow Island, Bassano and Medicine Hat. Add in the mental health therapists and psychologists, and the total mental health staff still only sits at 14.5 for the entire region. These professionals provide care to a population of over 100 thousand patients each year.
The Palliser PCN uses patient-reported outcome measures - like the PHQ-9 for depression and GAD-7 for anxiety - to track how well BHCs are helping patients. Patients fill these out once a year, giving a clear picture of their progress over time. This shows that people who see BHCs get better, use fewer emergency rooms, and are highly satisfied with the care they receive.
It’s cheaper, it’s faster, and it works.
But 8.5 FTE BHCs for an entire zone?
That’s not enough, we need more.
Why It Works (And Why It's Weird Here)
So, what makes them so great?
To me, it’s like talking to a friend who will keep your secrets (they are bound by strict privacy rules), a friend who is equipped to handle the heavy stuff.
But here is where things get tricky. And this is where the "Code Orange" part comes in.
In the Palliser zone, the way BHCs are funded is, frankly, odd. The funding model attaches these consultants to individual doctors. The doctor has to give up their own time and space in their practice to host the BHC creating a bottleneck. It means the number of BHCs available depends on how many doctors are willing and able to give up a room in their clinic. It feels like we are running a lifeboat service based on who happens to have a dock, rather than looking at the size of the ocean.
Our city saw the demand first-hand years ago when we had a cluster of men dying by suicide. My BHC called me to ask if we could reschedule my regular appointment, she needed that hour to see someone who had just lost a loved one in that cluster. I was happy to give up my spot.
There is another issue concerning BHCs - once upon a time - they were able to sign on for 3 year contracts, now the contracts are one year at a time. This causes uncertainty both for the BHCs and their clients.
We need more BHCs. We need them in every clinic, attached to every doctor, with a funding model that lets them focus on patients - not on fighting for office space.
How to Get Connected with a BHC in Palliser
Start with your family doctor. BHCs are attached to family physicians and or clinics in the Palliser Primary Care Network (Palliser PCN). Just ask your doctor at your next appointment if they have a BHC in their clinic, or if they can refer you to one.
Go to the Palliser PCN Website This link lists the BHCs and the clinics they are attached to.
If you're in crisis right now, don't wait for an appointment. Call the Mental Health Help Line at 1-877-303-2642 . It's free, confidential, and open 24/7. They can also connect you with local resources.
For children and youth, the Kids Help Line is always available at 1-800-668-6868.
If it's an emergency, if you or someone you love is in immediate danger,
call 911 or go to the nearest hospital. Help is there when you need it.
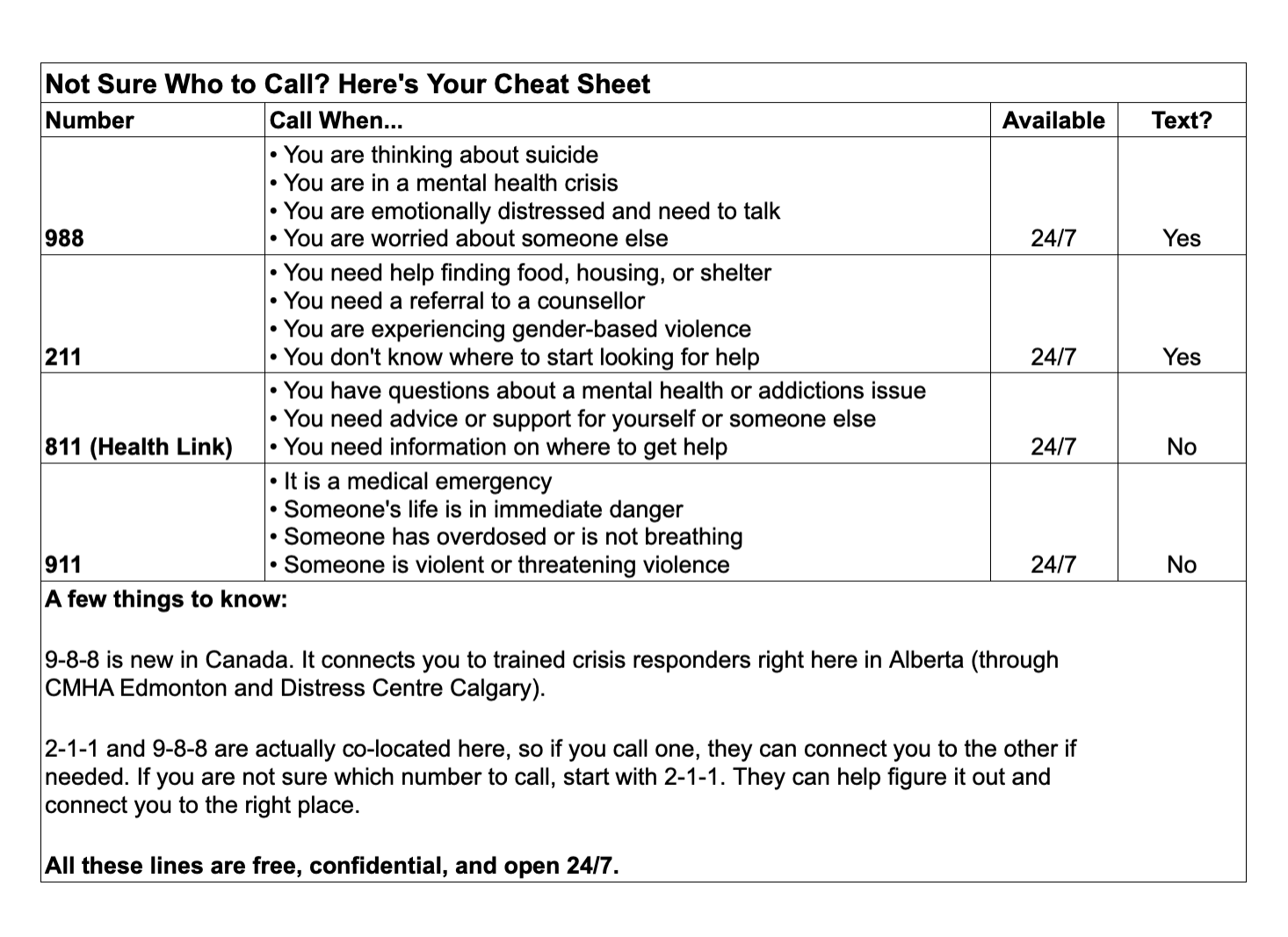
Next month is Stress Awareness Month. If you're feeling the weight of the world right now - political division, global conflict, caregiving - you’re not alone. This chart can help you know who to call.
Even if you call the wrong number, they can help guide you to the right resource.
Make the Call!
Created by Owl News
A peaceful South Saskatchewan River from Finlay Bridge, Medicine Hat, November 2025 - Photo by Kelly Allard